
Hip pain is common.
It shows up when you walk.
When you sit too long.
When you exercise.
Even when you’re trying to sleep.
You stretch.
You rest.
You Google exercises for pain in the hip joint.
Maybe it helps for a week. Then it comes back.
At Embody Health and Performance, we often find that hip pain isn’t about damage. It’s about how the body is moving, adapting, and compensating. The hip is rarely the villain. It’s usually the messenger.
Understanding that changes everything about how hip pain treatment should look.
Why Hip Pain Is So Common
To understand why hip pain treatment so often misses the mark, we first have to understand the role the hip actually plays in the body.
The hip sits at the center of the body. It connects your upper and lower halves. Every step, every squat, every transition from sitting to standing runs through it.
Your hip manages:
- Load
- Rotation
- Stability
- Force transfer between the trunk and legs
As a result, it is often the first place discomfort shows up when something else isn’t working well.
If your core isn’t supporting you well, the hip works harder.
If your ankle mobility is limited, the hip compensates.
If your spine isn’t rotating efficiently, the hip absorbs the extra demand.
Pain in the hip joint is often less about local injury and more about global stress.
Common Reasons We See Hip Pain at Embody
Once we understand how central the hip is, it becomes easier to see why discomfort shows up here so frequently.
Every body is different, but there are patterns we see consistently in hip therapy for pain.
Limited Hip Mobility (But Not Always Where You Think)
Yes, hips need mobility. Flexion, extension, and rotation all matter.
But tightness is not always the root problem. Sometimes what feels “tight” is actually a protective response to instability or poor load control.
In many cases, stretching alone may temporarily relieve discomfort including common movements like the kneeling hip flexor stretch. But if the underlying coordination or strength isn’t addressed, the tension often returns.
Mobility without control does not create resilience.
Core and Pelvic Support That’s Missing
In particular, we often see female lower back and hip pain connected to changes in pelvic support…
The hip does not function independently from the core or pelvic floor.
We often see female lower back and hip pain connected to changes in pelvic support, abdominal coordination, or postural strategies. Pregnancy, postpartum recovery, and hormonal shifts can all influence how load is managed through the pelvis.
When deep support systems are underperforming, the hip absorbs the excess demand.
Addressing hip pain treatment effectively means looking at how the entire lumbopelvic system is working together.
Overuse Without Enough Recovery
Sometimes the issue is not weakness. It’s accumulation.
You can be strong, active, and healthy — and still develop hip pain.
Long walks, new training programs, increased running mileage, or even repetitive daily standing can gradually exceed the hip’s current load tolerance.
The body adapts well. But it needs progressive exposure and adequate recovery to do so.
Compensation From Other Areas
We rarely treat the hip in isolation.
Limited ankle mobility can shift force upward.
Knee instability can increase hip compression.
Spinal stiffness can demand more rotation from the hip joint.
The hip often works overtime to keep you moving forward. Over time, that extra work shows up as pain.
The Hidden Cause of Lateral Hip Pain: It’s Not Always Bursitis
One of the most common examples of this misunderstanding shows up in lateral hip pain.
If you’ve ever felt aching pain on the outside of your hip, especially when walking, climbing stairs, or lying on your side, you may have been told it’s bursitis.
While hip bursitis does exist, lateral hip pain is not always true bursitis.
The bursa is a small, fluid-filled sac that reduces friction between tissues. When it becomes inflamed, it can cause pain. Because of this, lateral hip discomfort is often labeled as trochanteric bursitis.
This typically leads to:
- Rest
- Ice
- Anti-inflammatories
- Injections
- Avoiding activity
Sometimes these help temporarily. Often the pain returns.
Why?
Because the bursa is rarely the primary problem.
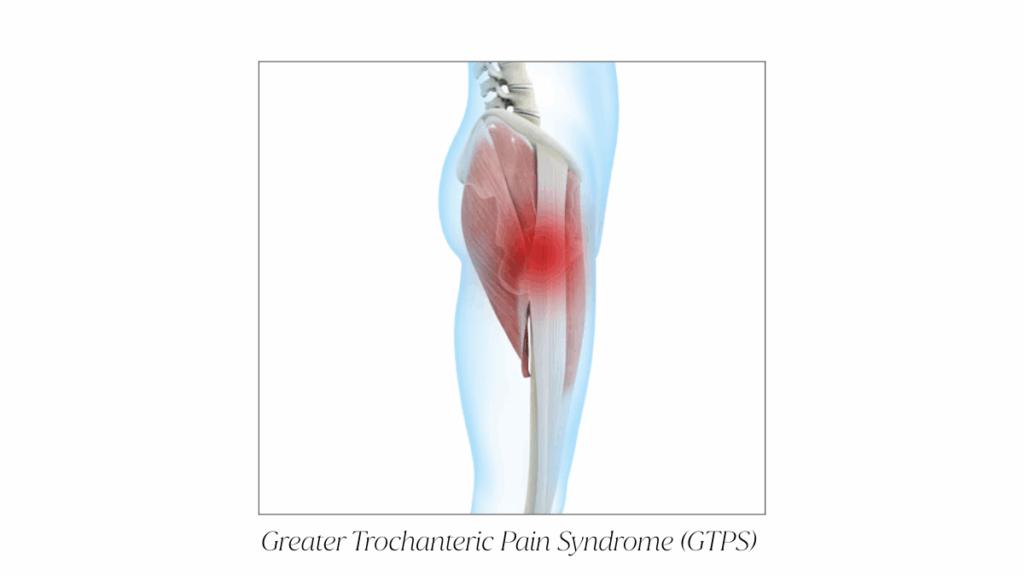
Most lateral hip pain falls under a broader category called Greater Trochanteric Pain Syndrome (GTPS). This includes:
- Gluteus medius and minimus tendon irritation
- Tendon degeneration
- Load intolerance of the lateral hip
- Secondary bursal irritation
In other words, the bursa is usually reacting to stress rather than creating it.
The most common underlying issue is poor hip stability and load control.
The gluteus medius plays a critical role in:
- Keeping the pelvis level during walking
- Controlling single-leg stance
- Stabilizing the hip during stairs and running
When it underperforms:
- The pelvis drops or shifts
- The hip experiences excessive compression
- Tendons become overloaded
- Pain develops gradually
This is why lateral hip pain often worsens with long walks, standing on one leg, side sleeping, or stairs.
Injections can reduce pain. They do not improve strength, coordination, or tendon capacity.
Rest calms symptoms. It does not retrain the system.
True hip joint pain physical therapy addresses strength, control, and progressive load tolerance.
Hip Pain Treatment That Looks Beyond the Joint
When we put these pieces together — mobility, stability, load, and compensation — a clearer picture of hip pain treatment begins to emerge.
Treating hip pain effectively means understanding how the entire body supports or overloads the hip.
At Embody, we look at movement before we look at muscles.
Movement Before Muscle Isolation
Isolated exercises have value. But they are rarely the starting point.
We assess how you walk, squat, rotate, and transfer weight. We look at coordination and timing, not just strength.
Hip pain treatment should restore patterns, not just target parts.
Strength That Builds Confidence
Avoiding movement entirely often prolongs the problem.
Instead of avoiding movement entirely, we use progressive loading to rebuild capacity safely. That means gradually reintroducing stress so the tissues adapt instead of flare.
Moving through manageable discomfort under guidance is different from pushing through pain blindly.
Confidence in movement matters.
Mobility That’s Purposeful
Stretching can help when it is applied intentionally.
A kneeling hip flexor stretch may be appropriate if true anterior hip restriction exists. But if the underlying issue is instability or load mismanagement, stretching alone can reinforce the problem.
Mobility must serve function.
Why Hip Pain Exercises Online Don’t Always Work
This is where many people get stuck.
You can find thousands of hip pain exercises online.
But they assume:
- The same cause
- The same movement history
- The same nervous system response
- The same tissue tolerance
That is rarely reality.
One-size-fits-all routines often miss the deeper pattern driving pain in the hip joint.
That’s why at Embody we assess movement patterns, not just symptoms.
When Hip Pain Keeps Coming Back
And if hip pain keeps returning, that repetition is not random.
More often than not, recurring hip pain is information.
It does not mean you are broken.
It does not mean you failed rehab.
It often means:
- Load exceeded current capacity
- Recovery was insufficient
- Stress levels changed
- Compensation patterns returned
Repeated flare-ups usually point to a bigger picture issue. Until that system is addressed, the cycle continues.
How Embody Approaches Hip Pain Differently
Because of this, our approach to hip therapy for pain is whole-body and individualized.
We focus on:
- Comprehensive movement assessment
- Identifying compensation patterns
- Strengthening support systems
- Educating you on load management
- Building long-term resilience
We do not chase symptoms.
We do not rely on passive treatments alone.
We build capacity.
The goal is not just pain reduction. The goal is sustainable function.
Final Thoughts: Your Hip Isn’t the Problem — It’s Part of the Story
Ultimately, hip pain makes more sense when we zoom out instead of narrowing in.
Hip pain is common. It is also often misunderstood.
Your body adapts constantly. Pain is usually a signal that the system needs recalibration, not that it is damaged beyond repair.
When you shift from treating the hip as the problem to understanding it as part of a larger movement story, progress becomes clearer.
If hip pain is limiting how you move or feel — and quick fixes haven’t helped — working with a physical therapist who looks at the whole body can change the trajectory entirely.
Explore Physical Therapy at Embody.
Learn About Our Approach.
Frequently Asked Questions About Hip Pain
Hip pain can be caused by joint irritation, tendon overload, muscle weakness, compensation from other areas like the spine or ankle, or changes in load and recovery. It is often multifactorial rather than a single structural issue.
No. Pain in the hip joint may actually be influenced by the lower back, pelvis, knees, or ankles. The hip frequently compensates for dysfunction elsewhere.
The hip and lower back share load and movement responsibilities. If one area underperforms, the other often compensates. This is especially common in female lower back and hip pain presentations.
Recurring hip pain often reflects incomplete load progression, unresolved compensation patterns, or changes in stress and recovery.